How to identify HPV-related lesions
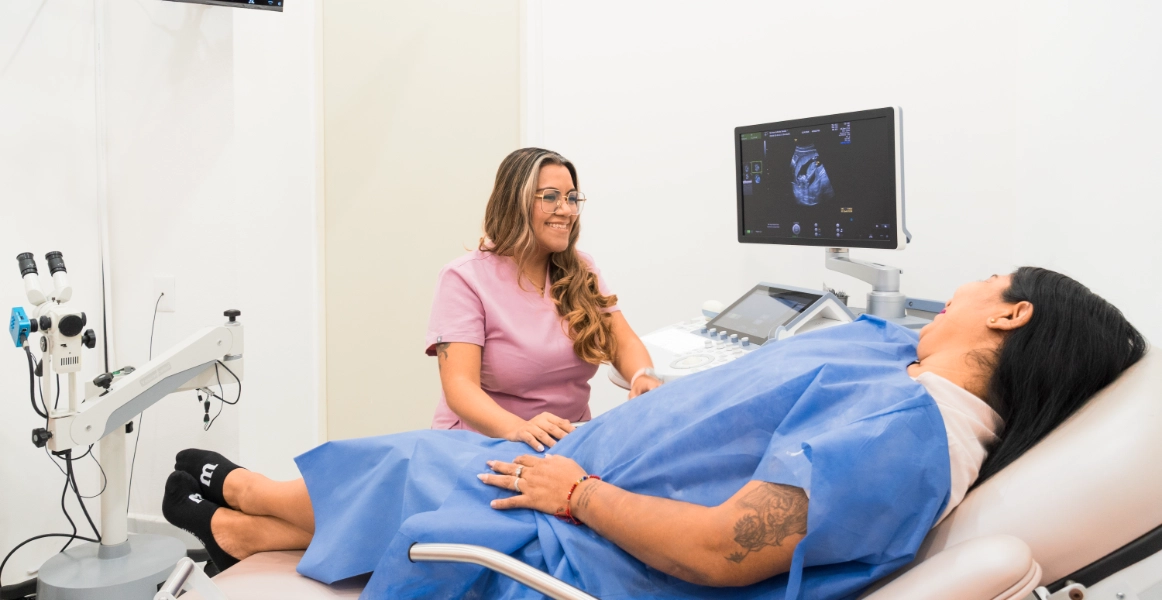
Some lesions may appear as small bumps, skin changes or warts in the vulva, vagina or anal region, but others are only detected during a gynecologic evaluation. Clinical examination helps distinguish between benign lesions, findings that require further testing and changes that should be monitored.
When clinically appropriate, a high-sensitivity HPV PCR test may be requested to identify high-risk genotypes and better define cervical follow-up. This test does not replace clinical evaluation: it is interpreted together with examination, Pap smear, colposcopy and medical history.
Prevention and follow-up
Condom use reduces the risk of transmission, although it does not eliminate it completely. Prevention also includes vaccination, periodic gynecologic checkups, Pap smear, colposcopy when indicated and timely follow-up to detect changes before they progress.
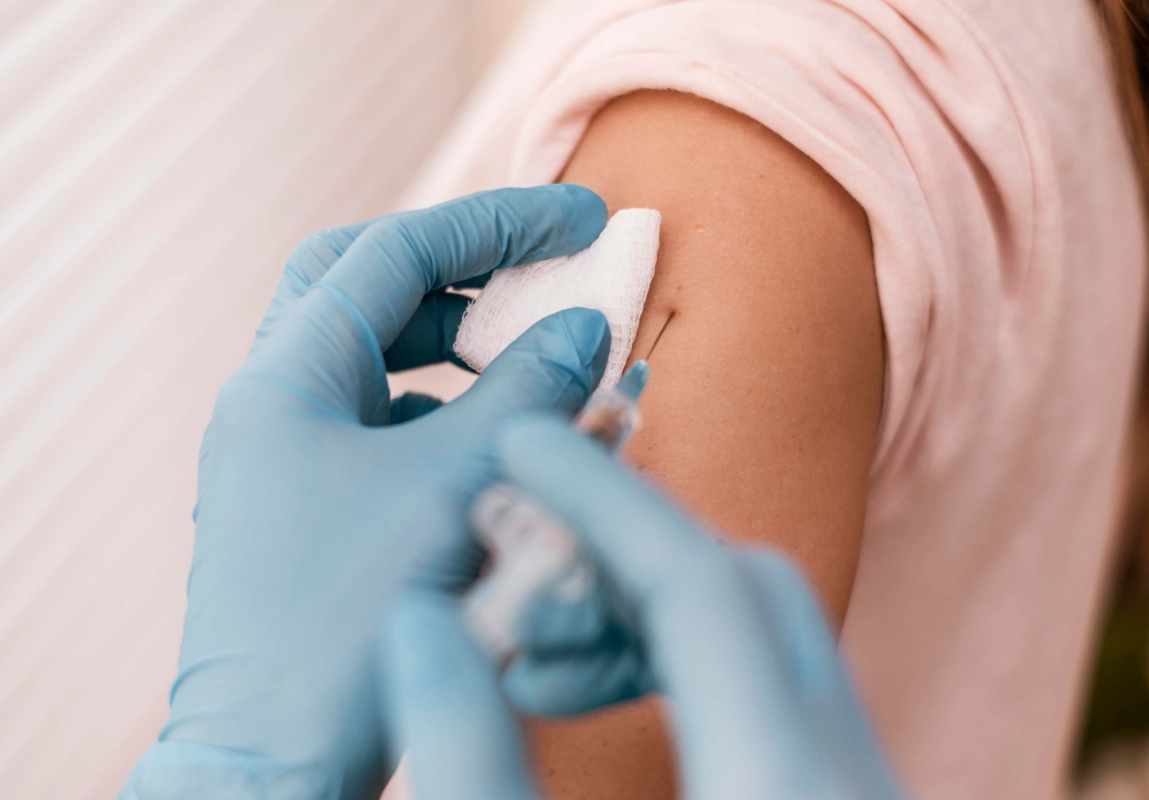
HPV vaccine
Vaccination is one of the best tools to lower the risk of infection from high-risk types and some HPV-related lesions. The recommended schedule depends on age and vaccination history. In consultation, we review whether it is still a good option in your case.
Common HPV questions
It depends on your age, previous results, whether visible lesions are present, Pap smear abnormalities or symptoms such as bleeding, burning or changes in the vulva or cervix. A gynecologic evaluation determines whether PCR, colposcopy or another study is needed.
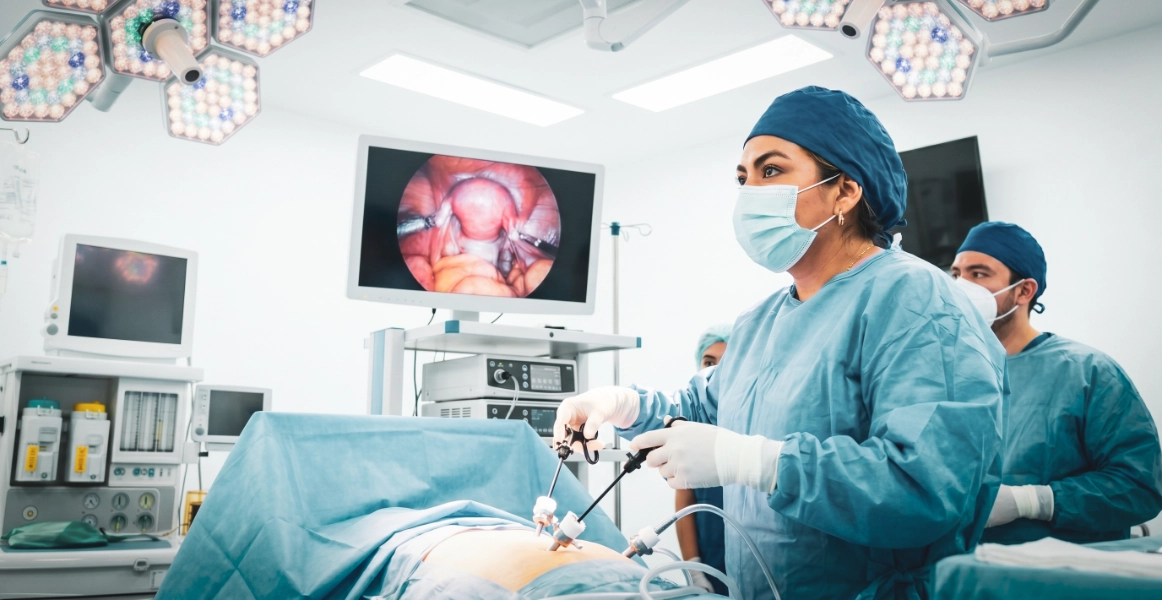
No. Some lesions only require observation, others can be managed with medication or local procedures, and selected warts may be treated with CO2 laser. The right approach depends on the type of lesion, its location and your clinical history.
In many cases, yes. Having had a previous infection does not mean you were exposed to all the types covered by the vaccine. The decision depends on age, prior infection history, current results and prevention goals.
Gynecologic consultation and gynecologic surgeries
Two frequent paths to start an evaluation or plan a procedure within the current catalog.